Childhood growth: A parent carer guide
Childhood growth: A parent carer guide
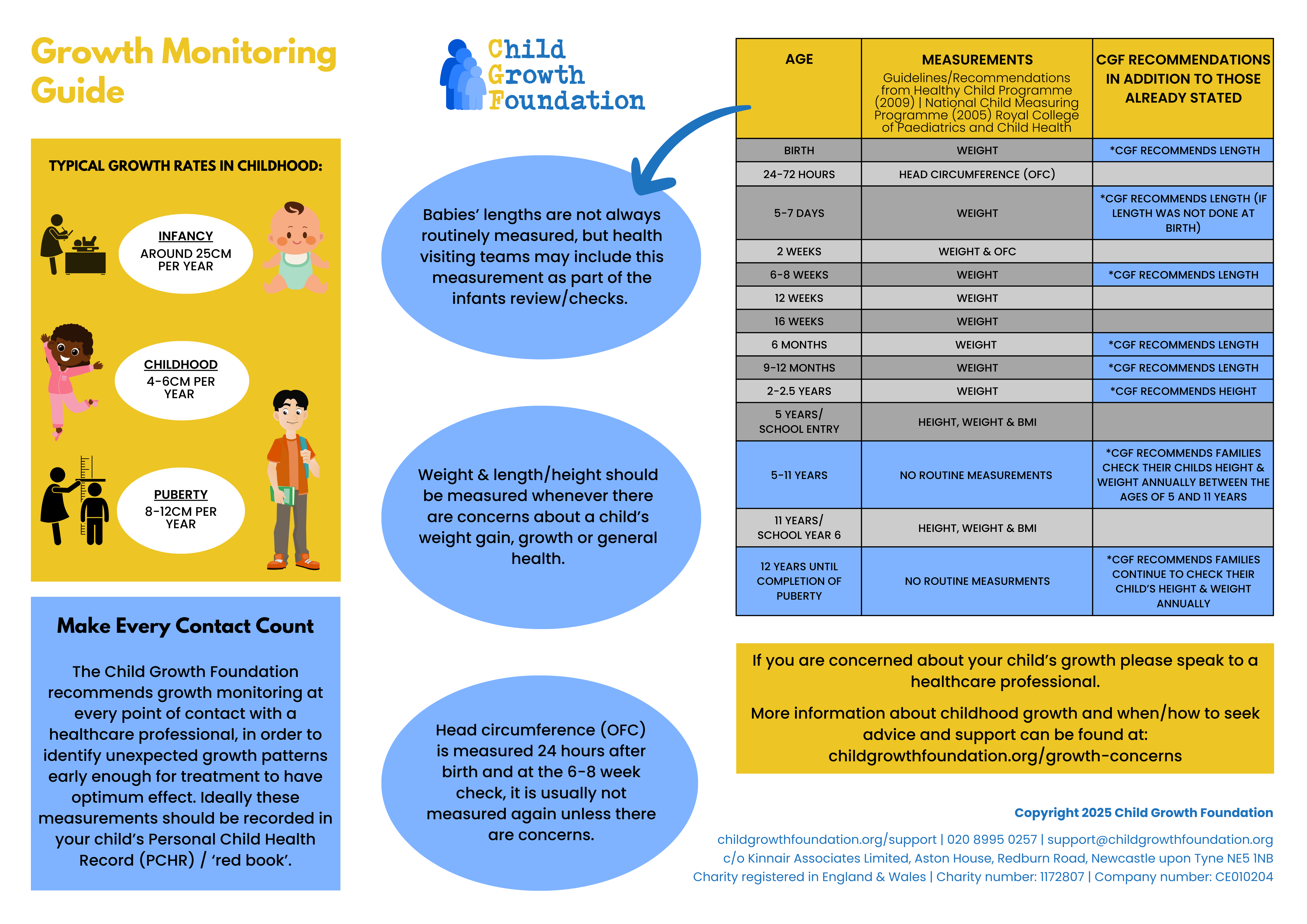
We’re delighted to share our new resource Childhood growth: A parent carer guide.
This guide is packed with information including typical growth in childhood and puberty, monitoring growth and measuring at home, head circumference measurements, concerns if you’re child is smaller or taller than expected, who to approach if you have concerns…and much more!
If you have questions or concerns about your child’s growth please speak to a healthcare professional, or contact our Support Line:
childgrowthfoundation.org/support | 020 8995 0257 | [email protected]
By contacting the Child Growth Foundation Support Line you are providing consent for us to collect, process and store your data to provide you with the information or services you are contacting us about. Read the full Support Line Privacy Statement at: childgrowthfoundation.org/supportlineprivacy