Michael’s Story
On the 30th March 2011, 11 weeks before his due date and weighing 820grams (1lb 13ozs), Michael made a dramatic entry into the world.
Two days earlier during a routine scan at Solihull hospital, the team discovered that Michael was not growing and probably hadn’t done so for two to three weeks due to an absent end-diastolic flow. I was immediately transferred to Heartlands hospital in Birmingham where they promptly diagnosed that I was suffering from Pre-eclampsia.
Following a forty-five minute emergency caesarean section operation performed by an eighteen person medical team led by Mr Mike Wyldes, Michael let out a small cry as he was delivered and ready for the fight that lay ahead. He was soon whisked away to the neonatal unit where he would take residence for sixty-eight days.
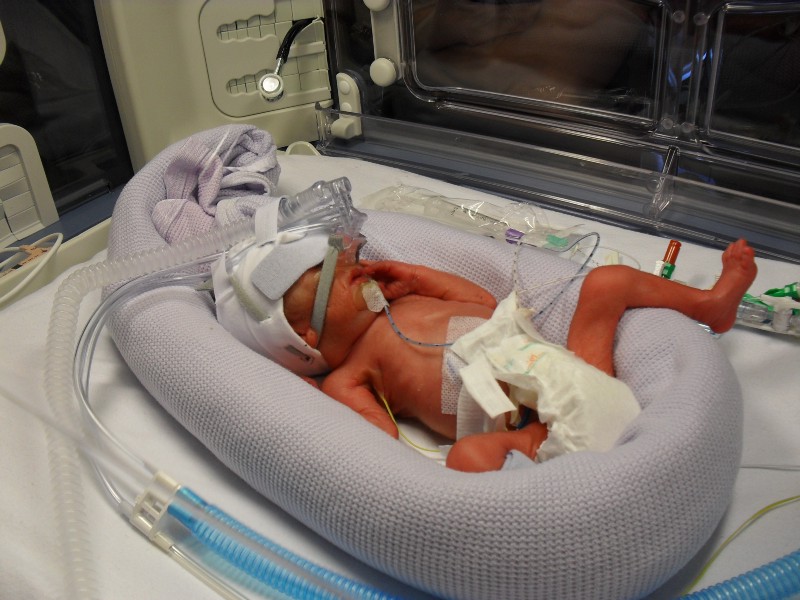
Michael was extremely strong, having been placed initially on CPAP to support his breathing as a precautionary measure, he was breathing by himself within twenty-four hours. My condition however, got progressively worse, being diagnosed with HELLP syndrome, my liver was failing and my blood was not clotting properly.
After 24 hours, my condition thankfully stabilised and once able to prove to the midwives that I could get out of bed unaided, I was allowed to go and see Michael. He appeared so fragile, his body covered in many wires and tubes. The nurses carefully took Michael out of the incubator and placed him on my chest for some Kangaroo Care (Skin to skin contact). This was to become a daily routine.
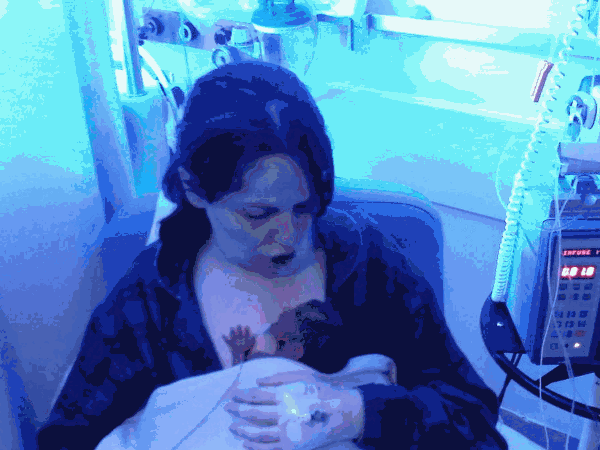
We were warned that a premature baby’s journey in Neonatal was akin to a rollercoaster. During the first week Michael did not tolerate breastmilk and had bile in his stomach. He was required to remain on Total Parental Nutrition (TPN) in which essential food is fed through long lines into a child’s body.
Two weeks after his birth, Michael started to tolerate milk and the Doctors decided that they would remove Michael’s TPN. Something was not right, I could see Michael’s heart rate increasing and his temperature rising on the monitors. Then Michael’s apnoea monitor sounded an alarm, Michael stopped breathing. Emma, the neonatal nurse gently rubbed his back and he started to breathe again. However, Michael stopped breathing again moments later, and having suspected an infection being caused from the TPN line, Emma had already summoned the doctor to assess Michael and address his condition. The Doctors and nurses immediately placed Michael back on to CPAP together with a course of antibiotics in order to fight the infection.
Michael needed to gain weight, this would be a slow process and was always commented upon by doctors during their rounds. Whilst in the incubator, Michael was fed breast milk which had been fortified. His weight soon increased, but once he weighed enough for a cot, his milk was no longer fortified. Unfortunately, whilst in the cot Michael actually lost weight and the hospital assigned a dietician who decided that Michael should consume High Energy SMA.
Michael began increasing in weight with this new milk and was finally discharged from the hospital. Whilst at home, Michael continued with High Energy SMA. Although not a great feeder and being sick often, Michael did put weight on, finally achieving the 25th Centile.

Weaning Michael was difficult and it was during this period we discovered he has quite a strong gag reflux. He would often be sick, even on pureed foods. We had to ensure Michael consumed the correct quantity of food so as to not be sick. Nappy bags soon became a great form of sick bag (and we still carry them around today!), sick bowls would be placed in several locations around the house in case of an emergency.
Michael’s Neonatal consultant closely monitored him, even though he was increasing in weight (albeit very gradually), his height was not increasing. We had always been informed that ‘catch up’ growth would probably happen in the first two years. Michael never caught up with his peers.
At eighteen months old, Michael was no longer taking high energy SMA and instead he was given Fortini supplements. This continued to make Michael sick so we took the decision to stop the supplements. Michael still had support from the dietician until the age of three, but as Michael was at least eating regular meals, the dieticians felt there was nothing further they could do.
When Michael was younger he struggled to fight off infections. When returning home from my first ‘back to work’ day, I noticed that Michael was struggling to breathe and I took him straight to the GP’s who advised to take him straight to A&E if his condition worsened. That night was spent in A&E (a winter was never a winter without a trip to A&E).
At three years of age, the Neonatal Consultant referred Michael to the Endocrinology team at Birmingham Children’s Hospital. We were really hoping that Michael would be discharged from his care (by this time all of the other children who I had met while Michael had been in hospital had been discharged). We never really questioned Michael’s growth before this, we knew he was smaller but there were some possible explanations. Firstly, Michael was born prematurely, secondly, both sets of grandparents are not particularly tall and thirdly we actually believed that he would ‘catch up’, he just needed time.
Michael’s initial Endocrinology appointment was fine, a decision was taken to measure his height accurately for 6 months so that the consultant could monitor him on a height velocity chart to understand his growth rate.
During the next appointment, I felt Michael had grown by less than one inch in 6 months. His health hadn’t been particularly great over the winter period. We discussed the next steps with the consultant and had to take the decision whether to start testing for growth hormone deficiency now or in 6 months time. We made the decision to start the testing right away.

The Stim test concluded that Michael was Growth Hormone Deficient, so a second test was arranged, the arginine test. The results of the second tests resulted in Michael being diagnosed as being Growth Hormone Deficient. On the 31st July 2015 Michael was injected with his first dose of growth hormone. The decision for growth hormone centred on wanting to give Michael an opportunity and if this did not work then we could be satisfied that this avenue had at least been explored.
The first three days were tough with many tears and tantrums. Honesty has been the best policy with Michael by explaining to him why he requires growth hormone. Michael is fantastic with the injections, taking all in his stride without a single complaint.
An MRI scan arranged by the Endocrine team discovered that Michael has a small pituitary gland.
Michael has now managed to be recorded on a growth line, although the 0.4th centile is was a level that he had never reached before. Michael’s health has dramatically improved, no sudden trips to A&E (touch wood) and no need for the frequent use of inhalers.
Michael’s weight is still of concern, having only gained three-and-a-half pounds in one year. We are trying to obtain another referral for a dietician and for a physiotherapist (as his gross motor skills are not at satisfactory levels, Michael struggles to push the pedals of a bike).
Michael is also being checked by a genetics team. A micro array test result was clear, the team are now testing for Russell Silver Syndrome.
Recently Michael had his first operation in which two cysts removed from his mouth. He was incredibly brave and the hospital were fantastic.
Michael is doing extremely well at school and he work very hard. However, he does often get frustrated with his peers because they are too young to realise that every one step of theirs requires two from Michael and all of the various medical appointments or tests that Michael has to endure. Other five year olds do not realise that by calling Michael ‘small’ or ‘a baby’, it affects him and he’ll ask ‘Am I getting bigger? ’.

Michael is now five years old and although he is currently diagnosed as being Growth Hormone Deficient, he is never disheartened and never gives up. A truly courageous and special little boy.







